When we met with the Department of Health’s new Permanent Secretary and his officials last week, one of my priorities was to make sure that they were left in no doubt about the impact of inflation and rising costs on dental practices in Northern Ireland.
Rising costs and declining incomes
We have prepared and presented a paper titled Rising Costs, which clearly outlines the problem. Dental treatment fees have been described by our MLAs as pittance. We can see this when comparing fees for an extraction and occlusal filling with a gel nail manicure, a haircut, a blow-dry and taking your dog to the vet.
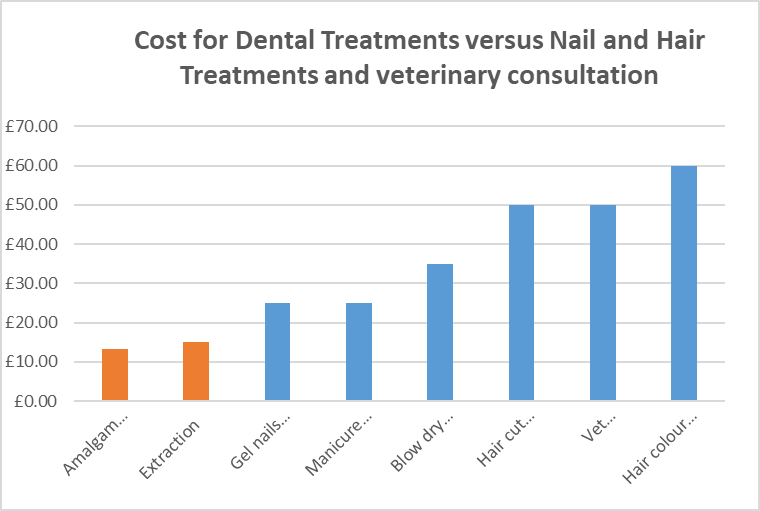
HS dentistry fees are set by the government and in the 30 years since the inception of the current contract, these fees have only increased marginally at sub-inflation rates. Not only have they not taken into account inflation, they have ignored the advances in and increased cost of dental technology and dental materials, the increased legislation within dentistry and the altered demographic and requirements of our population. The fees paid do not reflect the cost to provide care.
More investment is needed
There is a disconnect between the headline figure of how much is invested in dentistry, and what it translates to when it reaches an individual patient for an individual treatment. Regardless of how many millions are allocated for health service dentistry in Northern Ireland (£131.7m in 20/21), if it does not cover the costs to provide care and provide an adequate salary for the dental team, it is not enough.
Our research is based on real figures and real diaries. However, they were prepared by the BDA team and therefore do not constitute an independent body of work acceptable by the department as evidence of the need for additional investment.
If [investment] does not cover the costs to provide care and an adequate salary for the dental team, it is not enough.
We have therefore requested that the Department commission an independent report. It should be carried out by an accounting firm and a health economist to establish ‘average’ values for operating costs per surgery per day for a modern well-equipped practice and a time, treatment delivery, fees and costs study respectively. These studies will validate our figures and our repeated requests for the additional funding necessary to run a quality HS dental practice.
Inflation and HS dentistry in crisis
The advance of dental technology and materials and the current wider inflationary pressures mean that the costs associated with delivering HS dentistry in 2022 are soaring at a rapid pace. There is currently no mechanism in place to adequately offset these rising expenses and the detrimental impact they are having on independent contractors. We need a dental inflation indicator.
The stark reality is that health service dentistry is seriously underfunded and as a direct result, in crisis.
The creeping demise of health service dentistry in recent years has without doubt been accelerated by the pandemic to a point where it is unsustainable. The remuneration doesn’t even cover costs for several treatments – in particular dentures, bridges, crowns, extractions and simple occlusal fillings.
There persists a misguided perception that HS dentistry is a lucrative and rewarding profession. The stark reality in Northern Ireland in 2022 is that health service dentistry is seriously underfunded and as a direct result, in crisis.
The Department must find a way to address these rising costs and rebuild the GDS until the reform process around the new contract can be put in place. We understand that they face significant challenges. There are budgetary squeezes and fiscal policy pressures. But dentistry needs ‘levelling up’ to have a future, practitioners must be adequately recompensed for their time, skills, professionalism and costs. Only then, can oral health inequalities be meaningfully tackled.
Low wages make HS dentistry untenable
The Health Service is losing highly skilled dentists earlier and earlier in their career due to the low wages, high stress, high volume nature of the work created by the contract and level of funding. In a recent BDA NI survey, 92% of associates said they would not recommend a career in dentistry.
The Department of health needs to take urgent steps to prove to dentists and their teams that they are valued and have a future in NHS dentistry. Exiting the NHS is a one-way ticket, no-one ever goes back once they have left. They need to prevent the exodus now otherwise by the time a new contract is created, there will be no-one to deliver it.
Using real diaries, we calculated the average hourly rate of an associate dentist carrying out 100% health service dentistry and compared to other professions and trades.
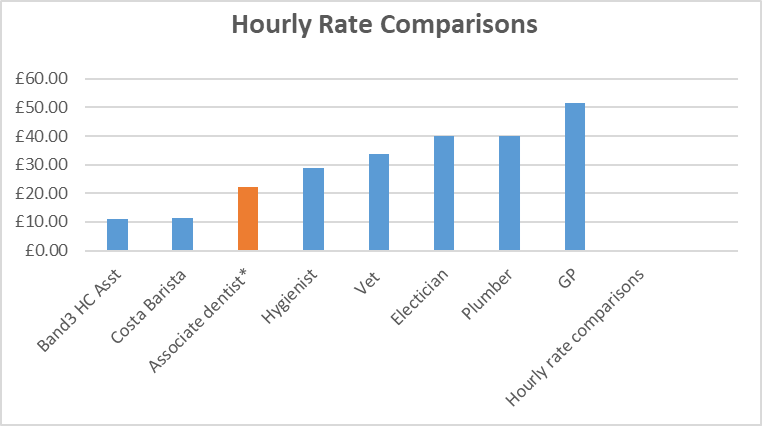
Looking at the stringent entry requirements, five years of intensive and expensive training, student debts to repay, plus the rigorous regulations and registration requirements. And then adding into the equation, the impact of inflation and the soaring cost of living that affects us all, it is clear that health service dentistry is far from an attractive career proposition.
While we progress our new contract negotiations, we have asked for the RSS enhancement to remain in place until then – or at least until the end of the financial year to allow some semblance of certainty – and to ease the impact of inflation.
The move towards private dentistry
In private dentistry, the fees charged to the patient reflect the costs to provide care. As costs rise, fees rise, this is a fundamental necessity to run a successful business. It is understandable that practices are reporting plans to increase the proportion of private care they provide in order to give them more time and the widest choice of materials and technology, whilst at the same time balancing their books.
The majority of practices in Northern Ireland are hybrid practices providing a mixture of NHS and private dentistry. The BDA exists to serve the needs of all members whatever their proportion of NHS and private. Indeed, our advice team spend much of their time providing advice to private and hybrid practices.
We will continue to negotiate with the Department of Health to fight for appropriate funding for HS dentistry, and in parallel we will provide the necessary advice for those who may be exploring diversifying more into private practice.
Ultimately, it is up to individual dentists and practices to find a way forward that works best for them and their patients in their unique circumstances. We will continue to campaign on behalf of all dentists and dentistry in Northern Ireland.

